What is Endometriosis?
Endometriosis is a medical condition characterized by the presence of endometrial-like tissue outside the uterus. This issue primarily affects the reproductive organs, including the ovaries, fallopian tubes, and the external surface of the uterus. As a result, tissue similar to the endometrium, which is the normal lining of the uterus, begins to grow in atypical locations. This abnormal growth can lead to chronic inflammation, pain, and a range of other reproductive challenges.
The condition is believed to affect approximately 10% to 15% of women of reproductive age, demonstrating its prevalence and significance in women’s health. Symptoms often include painful periods, pelvic pain, pain during intercourse, and challenges with fertility. However, the severity of these symptoms can vary significantly among individuals, making diagnosis particularly complex. Some women may experience mild symptoms, while others endure significant discomfort that can affect their quality of life.
Endometriosis not only causes physical symptoms but can also have emotional and psychological effects on individuals. The impact of the condition extends beyond physical discomfort, as struggles with infertility can create emotional strain. Women diagnosed with endometriosis often need support both medically and emotionally to manage this chronic condition effectively.
Understanding endometriosis is crucial for effective diagnosis and treatment. By recognizing its symptoms and implications, women can advocate for their health and seek medical guidance to address their specific needs. The condition is complex, and ongoing research continues to explore its causes and potential treatment options, improving outcomes for those affected.
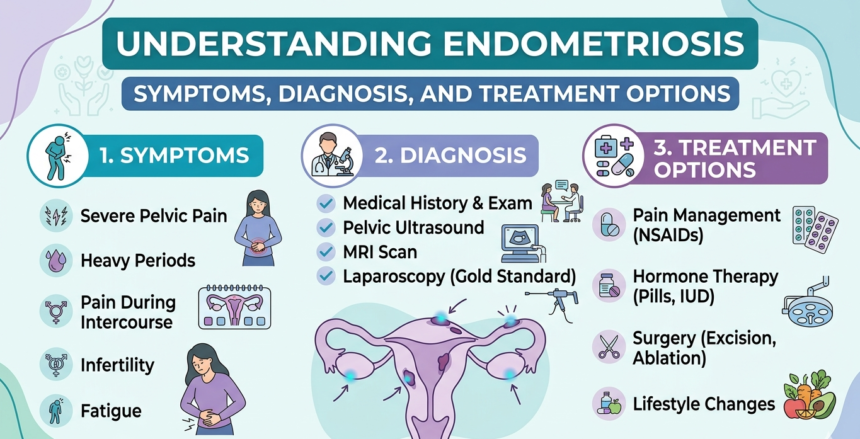
Common Symptoms of Endometriosis
Endometriosis is a chronic condition affecting millions of individuals, characterized by the growth of endometrial tissue outside the uterus. One of the most prevalent symptoms is pelvic pain, which often accompanies menstruation. This pain can range from mild discomfort to debilitating agony, severely affecting daily activities. Additionally, menstrual irregularities are commonly reported, including heavy bleeding (menorrhagia) or bleeding between periods, which can further complicate the diagnosis and management of the condition.
An alarming symptom associated with endometriosis is dyspareunia, or painful intercourse. Many individuals report discomfort during sexual activity, which may discourage intimacy and lead to emotional challenges. The emotional toll can be just as significant as the physical symptoms, as chronic pain and fertility concerns can affect mental well-being and relationships.
Other symptoms include gastrointestinal issues such as bloating, diarrhea, constipation, and nausea, often exacerbated during menstrual periods. These gastrointestinal symptoms can sometimes lead to misdiagnosis, as they mimic conditions like irritable bowel syndrome (IBS). Therefore, awareness of endometriosis symptoms is crucial, as they can vary greatly among individuals. Some may experience mild signs, while others endure severe manifestations that significantly hinder their quality of life.
It is also important to note that some individuals may remain asymptomatic or have symptoms that fluctuate over time, adding to the complexity of the disease. As such, understanding these symptoms and their variability is essential for early detection and appropriate treatment, enhancing the chances for effective management and improved well-being for those affected by endometriosis.
How is Endometriosis Diagnosed?
Diagnosing endometriosis can be a complex and multifaceted process, requiring thorough evaluation and various techniques to confirm the presence of this condition. The first step typically involves a detailed patient history, where healthcare providers gather information about symptoms, menstrual cycles, and family history of endometriosis. This initial assessment is crucial, as it helps identify patterns and possible connections that might indicate the prevalence of the disorder.
Following the history-taking, a pelvic examination is often performed. During this exam, a physician may check for abnormalities such as tender areas, cysts, or nodules, particularly in the pelvic region. Although a pelvic exam alone cannot definitively diagnose endometriosis, it may provide additional clues that warrant further investigation.
Imaging techniques are vital tools in the diagnostic process. Ultrasounds and Magnetic Resonance Imaging (MRI) are commonly employed to visualize internal structures and identify potential endometrial implants or cysts on the ovaries. An ultrasound can reveal ovarian endometriomas, while an MRI is particularly useful for mapping larger endometrial growths or lesions that may not be apparent on ultrasound. However, it is important to note that while these imaging methods can suggest the presence of endometriosis, they cannot confirm it. This leads to the necessity of additional diagnostic procedures.
The gold standard for confirming endometriosis remains laparoscopic surgery. This minimally invasive procedure allows the physician to directly view the pelvic organs and take samples of tissue, which can then be analyzed histologically. While laparoscopy is highly effective in diagnosing endometriosis, it does carry risks, including complications related to anesthesia and potential surgical issues. The challenges surrounding the diagnosis often stem from the variability in symptoms, as some women may experience severe pain while others remain asymptomatic. Consequently, delayed diagnosis is common, impacting access to timely treatment.
The Potential Causes of Endometriosis
Endometriosis is a complex condition that affects a significant number of women worldwide, and understanding its potential causes is essential for effective diagnosis and treatment. While the exact reasons behind endometriosis remain unclear, several theories have emerged outlining various genetic, hormonal, immunological, and environmental factors that may contribute to its development.
Firstly, genetic predisposition is a commonly cited factor in the onset of endometriosis. Women who have a family history of the condition are at a higher risk of developing it themselves. Researchers have identified certain genes that may increase susceptibility, suggesting that hereditary factors might play a crucial role in its pathogenesis.
Hormonal influences, particularly the role of estrogen, are also integral to understanding endometriosis. Estrogen promotes the growth of endometrial tissue, and elevated levels of this hormone have been observed in women suffering from endometriosis. This has led to speculation that hormonal imbalances could trigger the ectopic growth of endometrial tissues outside the uterus, resulting in the symptoms associated with the condition.
Immunological aspects have gained attention as well, with abnormalities in the immune system being proposed as another potential cause of endometriosis. It is suggested that a compromised immune response could fail to identify and eliminate ectopic endometrial cells, allowing them to thrive and cause inflammation and pain.
Finally, environmental factors may also contribute to the risk of developing endometriosis. Exposure to certain chemicals, toxins, and endocrine disruptors in the environment could play a role in the observed incidence rates. Consequently, ongoing research aims to identify specific environmental influences that may be linked to endometriosis.
Impact of Endometriosis on Daily Life
Endometriosis is a chronic condition that profoundly influences the daily lives of those affected. The physical manifestations of this disease can significantly hinder an individual’s ability to engage in routine activities. Common symptoms such as pelvic pain, heavy menstruation, and fatigue can lead to frequent absences from work or school. These disruptions can result in a decreased quality of life, making it challenging for individuals to maintain consistent schedules.
In addition to physical challenges, the mental health repercussions of endometriosis cannot be overlooked. Many individuals report experiencing anxiety, depression, and feelings of isolation. The uncertainty surrounding the condition and its symptoms can contribute to stress and a sense of helplessness. The chronic nature of this illness can lead to frustration, not only due to the pain experienced but also because of the societal misconceptions that often accompany the condition. This aspect of living with endometriosis necessitates greater awareness and understanding from family, friends, and the community at large.
The impact on relationships is another important consideration. Individuals may struggle to communicate their experiences and needs to partners, leading to misunderstandings and strain. It is essential for those living with endometriosis to have supportive networks that encourage open dialogue. By fostering understanding among friends and family members, individuals can not only alleviate some of the emotional burden but also navigate their relationships more effectively.
Lastly, endometriosis can severely affect one’s ability to pursue career opportunities or educational goals. The persistent pain and associated symptoms may force individuals to make hard choices about their professional aspirations, inadvertently limiting their potential. It is vital for employers and educational institutions to recognize these challenges and provide accommodations that can help those with endometriosis thrive.
Conventional Treatment Options for Endometriosis
Conventional treatment options for endometriosis aim to alleviate pain, manage symptoms, and address the hormonal factors contributing to the condition. The three primary treatment modalities include pain management strategies, hormonal therapies, and surgical interventions, each serving a specific purpose depending on the severity of the symptoms and the individual patient’s needs.
Pain management is often the first line of defense against endometriosis-related discomfort. Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen and naproxen, are commonly used to reduce pain and inflammation associated with this condition. These medications are generally effective and can be obtained over-the-counter, providing immediate relief for patients experiencing acute pain.
Hormonal therapies are designed to adjust the body’s hormonal balance, which may help slow the growth of endometrial tissue and alleviate symptoms. Common options include hormonal contraceptives, such as birth control pills, which regulate menstrual cycles and can decrease menstrual flow and pain. Additionally, other hormonal treatments like GnRH agonists can induce a temporary menopause-like state, significantly reducing pain and endometrial lesions. However, it’s crucial to consider potential side effects, like bone density loss and hormonal fluctuations, which may influence patient choice.
Surgical options are typically recommended for more severe cases of endometriosis, especially when other treatments fail to provide adequate relief. Laparoscopy, a minimally invasive procedure, allows for the removal of endometrial patches and adhesions. For some women, a hysterectomy might be considered as a definitive solution, particularly in cases where fertility is not a concern. While surgery can greatly reduce symptoms, it carries inherent risks associated with any surgical procedure.
In summary, treatment for endometriosis is multifaceted, involving a combination of pain relief, hormonal regulation, and surgery when necessary. Each approach has its benefits and potential downsides, making individualized treatment essential for effective management of this complex condition.
Alternative and Complementary Therapies
Individuals diagnosed with endometriosis often seek alternative and complementary therapies to manage their symptoms, as conventional medical treatments may not fully address their needs. These approaches can significantly contribute to enhancing overall well-being and alleviating discomfort associated with endometriosis.
One widely explored area is dietary changes. Some individuals find success in following an anti-inflammatory diet, which includes whole foods rich in antioxidants and omega-3 fatty acids. Such dietary choices may help reduce inflammation and mitigate symptoms, although scientific evidence on the effectiveness of specific diets remains inconclusive.
Acupuncture, a traditional Chinese medicine practice, is another complementary option. Studies suggest that acupuncture may help in reducing pelvic pain and improving the quality of life for endometriosis patients. Its ability to enhance blood flow and decrease stress can be particularly beneficial, although results can vary based on individual circumstances.
Physical therapy, particularly pelvic floor therapy, can also play a vital role in managing endometriosis symptoms. This form of therapy focuses on relieving muscle tension and restoring normal pelvic function. Many patients report improved mobility and a reduction in pain following treatment, indicating its potential efficacy as a complementary approach.
Mindfulness practices, such as yoga and meditation, are increasingly recognized for their stress-relief benefits. These techniques may alleviate chronic pain by promoting relaxation and bodily awareness. Although research is still emerging, some evidence suggests that regular practice can improve mental well-being for those dealing with endometriosis.
While exploring these alternative therapies, it remains crucial for individuals to consult with healthcare providers. Integrating complementary treatments should be done under professional guidance to ensure safety and effectiveness, thereby creating a holistic plan tailored to the individual’s specific needs.
Living with Endometriosis: Tips and Strategies
Endometriosis can significantly impact daily life, both physically and emotionally. Managing the symptoms effectively requires a multifaceted approach. One of the primary strategies is to maintain a symptom diary. Tracking symptoms, dietary habits, and menstrual cycles can help patients identify triggers and patterns, thus enabling more informed discussions with healthcare providers.
Incorporating a healthy lifestyle can also play a pivotal role in managing endometriosis symptoms. Regular physical activity, such as yoga or low-impact exercises, can help alleviate pelvic pain and improve overall well-being. Additionally, a balanced diet rich in anti-inflammatory foods, including fruits, vegetables, whole grains, and omega-3 fatty acids, may help reduce inflammation and hormonal fluctuations that can exacerbate symptoms.
Maintaining emotional health is equally important. Practicing mindfulness techniques, such as meditation or deep-breathing exercises, can help reduce stress levels associated with living with endometriosis. Furthermore, engaging in hobbies or activities that bring joy can serve as a distraction from pain and anxiety.
Building a robust support network is vital for individuals living with endometriosis. Communicating with friends, family, or a support group can provide emotional reinforcement and practical advice. Connecting with others who share similar experiences fosters understanding and reduces feelings of isolation, which can accompany chronic conditions.
Lastly, it is crucial to regularly consult with healthcare professionals to ensure the management strategies align with personal health goals. Individualized care plans can enhance treatment effectiveness and quality of life. By employing these tips and strategies, those affected by endometriosis can work towards a more manageable and fulfilling existence.
Future Research and Perspectives on Endometriosis
Research into endometriosis has significantly progressed over the past few decades, but many aspects of the condition remain poorly understood. Ongoing studies aim to uncover the biological mechanisms underlying endometriosis, including the role of genetics, hormonal influences, and immune system interactions. These insights could lead to better diagnostic tools and therapeutic options for individuals suffering from this complex condition.
Emerging treatments for endometriosis are at the forefront of current research. Clinical trials are exploring novel pharmacological agents, such as selective estrogen receptor modulators and anti-inflammatory drugs, which aim to alleviate symptoms with fewer side effects compared to conventional therapies. Additionally, advancements in minimally invasive surgical techniques continue to enhance the effectiveness of treatment while reducing recovery time. As researchers delve deeper into the pathophysiology of endometriosis, personalized medicine approaches are anticipated, tailoring treatment strategies to the unique presentation of the disease in each patient.
Advocacy and awareness play a crucial role in the future of endometriosis research. Increasing public knowledge about the condition can facilitate earlier diagnoses, promote funding opportunities, and enhance support networks for those affected. Continued partnerships between healthcare providers, researchers, and advocacy groups are essential to create an inclusive environment that highlights the importance of endometriosis. Furthermore, addressing the stigma around reproductive health issues encourages open discussions, paving the way for more comprehensive research.
In conclusion, the landscape of endometriosis research is continuously evolving, with a focus on innovative treatments, heightened awareness, and collaborative efforts to improve patient outcomes. Ongoing investigation into this complex condition promises to offer hope for affected individuals, potentially transforming the way endometriosis is managed and understood.